News
Veterans Booklet
Immunisation Schedule Change - 1st July 2025
Op Restore
Op RESTORE, The Veterans Physical Health & Wellbeing Service is for anyone who has served at least one day in HM Armed Forces and who have continuing physical health injuries or related medical problems attributed to their time in the Armed Forces. It is for both former
regulars and reservists.
Op RESTORE uses a network of civilian and military consultants, along with welfare support from military charities, to support a veteran’s health using a holistic approach. Once the referral is received from the GP practice, the veteran will receive a text from the service to book a call with a member of the Op RESTORE team who is themself a member of the Armed Forces Community. During the call they will check exactly what the veteran wants to achieve from the referral and identify any wellbeing needs. Any identified needs will either be supported by the Navigator, or by Support Workers at Defence Medical Welfare Services (DMWS).
All these issues will be discussed in a consultant-led multidisciplinary team meeting that will confirm the best clinical pathway and initiate that. The veteran will be kept informed throughout with a text message with a copy of the outcome letter and the offer of a follow up phone call. The GP practice will also receive the outcome letter, so they are kept in the loop. The veteran will be supported throughout the rest of their clinical care by the team.
Whilst Op RESTORE cannot shorten NHS waiting times, it seeks to ensure the veteran has all their needs, both health related and other, dealt with as effectively as possible.
For further information please contact us via https://www.imperial.nhs.uk/our-services/oprestore
New NHS Weight Management Medication Update
The medication Tirzepatide brand name (Mounjaro®) is being made available on the NHS for eligible patients across the UK, including Dorset.
The NHS locally is developing new services to allow GPs or other services in primary care to prescribe weight loss medications to those with a BMI over 40 with 4 associated conditions.
Around 1,000 people in Dorset are expected to qualify based on this national criteria.
However, it won't be available locally until Autumn 2025, so please don’t contact the practice yet—we’re not able to help with this currently.
For the latest local updates, visit the NHS Dorset website here>>
Notice
We are currently sending out information by text message.
For longer messages you may receive the information below.
Please be advised this is a safe link to use.
'You have received an important message from The Birchwood Practice. In order to view please click on the link. Many thanks.'
Once you have clicked on the link you will be asked to enter your date of birth and the access code number which you will find at the end of your text message.
Best regards
The Birchwood Practice
Change of Personal Details

We would like to invite you to use the NHS APP
The new simple and secure way to access a range of NHS Services on your smartphone or tablet
Use the NHS App to:
- check your symptoms
- find out what to do when you need help urgently
- book and manage appointments at your GP surgery
- order repeat prescriptions
- view your GP medical record securely
- register to be an organ donor
- choose how the NHS uses your data
Connecting GP surgeries to the NHS App
Patients at 95% of GP surgeries in England can now use all the features of the NHS App.
You can check if your GP surgery is connected when you open the app for the first time. If it's not, you can register your email address, and we'll notify you when they go live.
If your GP surgery is not connected, you can still download the app and use it to check your symptoms and find out what to do when you need help urgently.
Keeping your data secure
When your surgery is connected, and you register in the app, we'll carry out checks to confirm your identity. The app will then securely connect to information from your GP surgery. To keep your access secure, we'll send a security code to your phone each time you use the app.
Register with the NHS app: Quick guide (youtube.com)
MMR Vaccination
There is currently a National MMR (Measles, Mumps & Rubella) Vaccination/Immunisation Catch up Campaign. Therefore, anyone from the age of 12 months up to and including 25 years of age, will be contacted over the next couple of months if they haven’t had a complete course. You will be asked to contact your surgery and book an appointment with a nurse for the outstanding immunisation.
Should you need any further information, please click on the following link:
MMR for all: general leaflet - GOV.UK (www.gov.uk)
Quit Smoking
If you are thinking of Quitting heres some useful information that may help you

Adult Social Care
We are currently promoting Adult Social Care within our surgery. Take a look below to see what this could mean for you! Have a read of our factsheets and browse through our directory.
Factsheets – www.bcpcouncil.gov.uk/ascfactsheets
Service Directory – www.bcpcouncil.gov.uk/ascservicedirectory
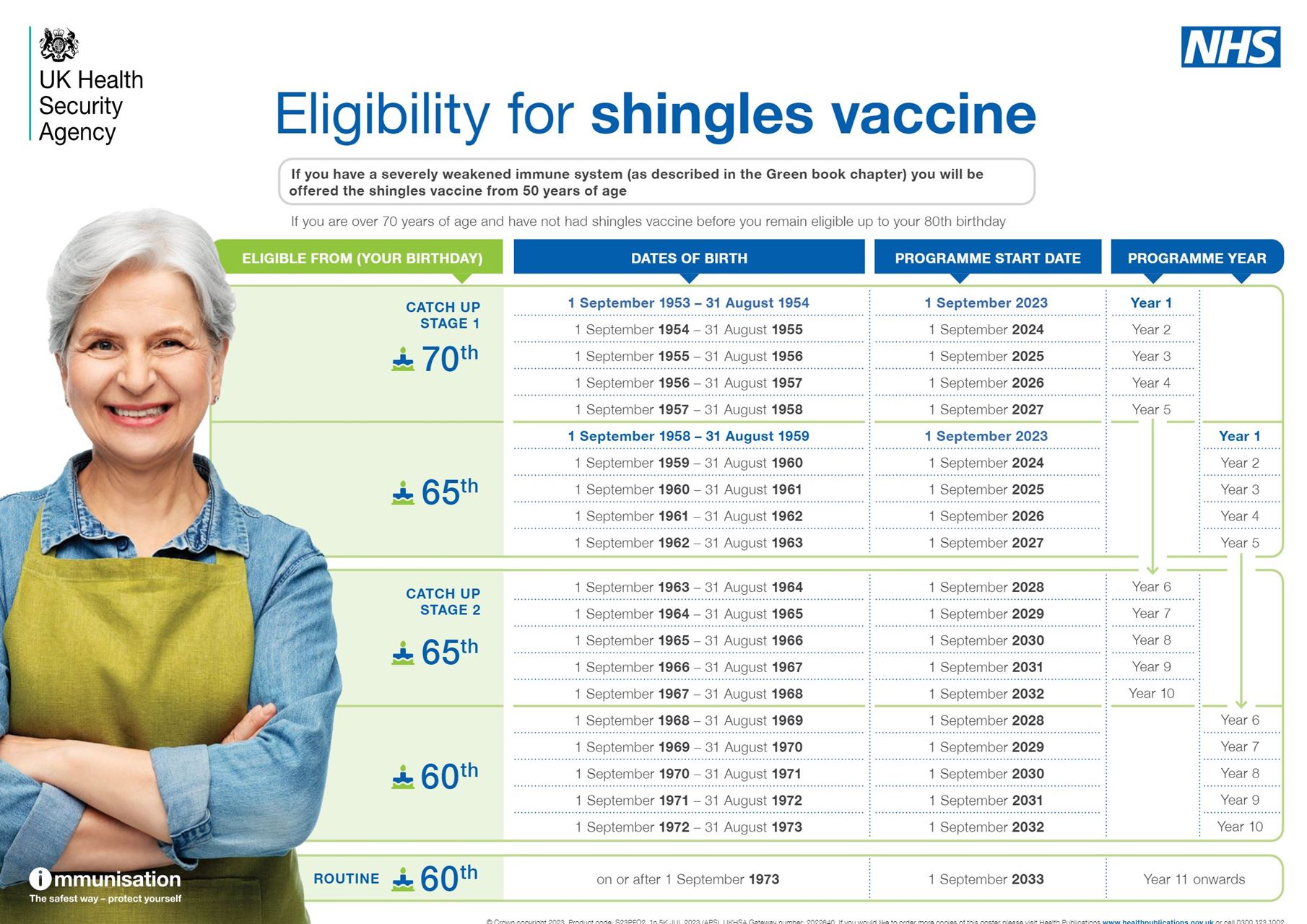

Shingles Eligibility
Shingles Eligibility
People aged 50 and over with a severely weakened immune system
You're eligible for the shingles vaccine if you're aged 50 or over and you're at higher risk from shingles because you have a severely weakened immune system.
This includes:
- some people with blood cancer (such as leukaemia or lymphoma)
- some people with HIV or AIDS
- some people who've recently had a stem cell transplant, radiotherapy, chemotherapy or an organ transplant
- people taking certain medicines that severely weaken the immune system
You'll be given 2 doses of the shingles vaccine. These are given between 8 weeks and 6 months apart.
People who turn 65 on or after 1 September 2023
- From 1 September 2023, you're eligible for the shingles vaccine when you turn 65.
- You'll be offered 2 doses of the vaccine. These are given between 6 and 12 months apart.
- You'll remain eligible until your 80th birthday.
If you turned 65 before 1 September 2023, you'll be eligible for the shingles vaccine when you turn 70.
People aged 70 to 79
- Everyone aged 70 to 79 is eligible for the shingles vaccine.
- Depending on the type of vaccine you have, you'll have either 1 dose or 2 doses (given between 6 and 12 months apart)
- You're eligible up until your 80th birthday.
Pneumococcal Vaccine
We are sending out messages to all our patients who are eligible for the Pneumococcal Vaccine which protects against serious and potentially fatal pneumococcal infections. Its also known as the Pneumonia Vaccine.
Please follow the useful link below for further information on the vaccine and who is eligible.
PneumoAware | Pneumococcal infection awareness | MSD
Healthy Steps Programme is Launching!
|

Extended Health Care Team
We are happy to help with all these services with the exception of Physician Associate or paramedic
updated Early Years Handbook

Change of Personal Details

FREE NHS HEALTH CHECKS
We are inviting patients who are between the ages of 40 and 74 to attend for their Free NHS Health check. Health checks are being offered to people aged between 40 and 74 once every five years.
Invites will be sent out in your birthday month and we will contact you either by phone, MJOG or letter.
The check should take about 20-30 minute and is based on straightforward questions and measurements.
WHAT HAPPENS AT THE CHECK
- You will be asked some simple questions about your family history and choices which may put your health at risk
- We will check your blood pressure and cholesterol
- We’ll record your height, weight, age sex and ethnicity
- You will receive general advice about what you can do to stay healthy.
Even if you are feeling well, its worth having your NHS Health Check – for more information please click on the link www.nhs.uk/nhshealthcheck to find out more information.
Thank you
Birchwood Practice
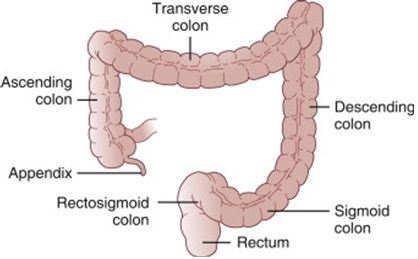
Bowel Cancer Screening
Weight Management Clinic
The Birchwood Practice is pleased to be offering a free new Weight Management clinic, this is open to all our eligible patients. In the clinic you will be seen by our HCA where your height and weight will be taken and then if eligible you will be signposted for further help.
This new programme provides an alternative way of accessing weight management support and will help you explore the different options available to you which will enable you to acheive your desired goals.

weight management
BREAST SCREENING
Dorset Breast Screening Unit will soon be contacting all our eligible women patients to invite them to book their Breast Screening appointment. We recommend that you take up this screening opportunity as detection of early abnormalities can prevent life threatening disease. For further information visit: Breast Screening Unit (uhd.nhs.uk)

Community Connector Volunteers
We are looking for ‘Community Connector’ volunteers to support people in the community and help reduce loneliness and social isolation.
Community Connectors are volunteers who will visit a person in their home a few times before accompanying them to activities until they feel happy to attend independently.
You will be helping people to:
- Find out about local community services and activities
- Participate in new activities
- Build new friendships, reduce loneliness and feel more positive
If you would like to find out more please visit Poole Community Action Network on https://www.can100.org/pages/category/a-good-life
We are offering training for those interested. If you would like to become a volunteer or would like to find out more please email contact.poolenorth@nhs.net
IT Help is Available
|

General Practice Data for Planning and Research - Update
Patient data from general practice has significantly contributed to the improvement of health and care services and treatments for many years. Patients rightly trust their GP to safeguard their data, a role that we know that all general practitioners take very seriously. This is why I am writing to share more information with you about how we are working to improve how this data is collected.
NHS Digital is making improvements to how data is collected from general practice, with a new framework for data extraction called the General Practice Data for Planning and Research (GPDPR) collection.
You will have seen the announcement to pause the collection of this data, to provide more time to engage with GPs, patients, health charities and others, and to strengthen the plan.
We are working in collaboration with a range of partners including the Royal College of General Practitioners (RCGP) and the British Medical Association (BMA). I want to reassure you that we have heard your concerns loud and clear and will continue to listen.
I am writing now to provide an update on the four key areas of work to strengthen the plan. We hope this will foster your trust in the system and provide a strong basis for you and your patients to participate in the scheme with confidence.
Most importantly, I can confirm today that, while we are continuing to work on the infrastructure, and communication for the project, we are not setting a specific start date for the collection of data. Instead, we commit to start uploading data only when we have the following in place:
● the ability to delete data if patients choose to opt-out of sharing their GP data with NHS Digital, even if this is after their data has been uploaded;
● the backlog of opt-outs has been fully cleared;
● a Trusted Research Environment has been developed and implemented in NHS Digital;
● patients have been made more aware of the scheme through a campaign of engagement and communication.
In this letter each of these adjustments are set out, all of which are critical to the success and impact of the programme, including through better understanding of the huge benefits the programme will have to the NHS and to our ability to provide the best and safest possible care for patients.
Opt-outs
We want to make the position around opt-out much simpler. While 1st September has been seen by some as a cut-off date for opt-out, after which data extraction would begin, I want to reassure you that this will not be the case and data extraction will not commence until we have met the tests.
We are introducing three changes to the opt-out system which mean that patients will be able to change their opt-out status at any time:
- Patients do not need to register a Type 1 opt-out by 1st September to ensure their GP data will not be uploaded;
- NHS Digital will create the technical means to allow GP data that has previously been uploaded to the system via the GPDPR collection to be deleted when someone registers a Type 1 opt-out;
- The plan to retire Type 1 opt-outs will be deferred for at least 12 months while we get the new arrangements up and running, and will not be implemented without consultation with the RCGP, the BMA and the National Data Guardian
Together, these changes mean that patients can have confidence that they will have the ability to opt-in or opt-out of the system, and that the dataset will always reflect their current preference. And we will ensure it is easy for them to exercise the choice to opt-out.
Administrative workload
We have heard from many GPs and practices that there is concern about the administrative burden that Type 1 opt-outs have placed on you and your teams. We are in the process of working with colleagues across general practice to develop a way of simplifying and centralising the opt-out process in order to remove this burden on practices. This is still in development, but we will share further information with you in the coming weeks.
In the meantime, given the changes we have agreed to the opt-outs there is now no urgency to process Type 1 opt-outs specifically for GPDPR in order to get people opted out before September. We will keep you updated on timelines for when we expect the programme to go live.
We will also ensure that the NHS Digital Data Protection Impact Assessment (DPIA) reflecting these changes to the programme is published well before data collection commences. A template DPIA for practice use will also be made available in good time to allow practices to complete it.
Data Security and Governance
The Government has committed that access to GP data will only be via a Trusted Research Environment (TRE) and never copied or shipped outside the NHS secure environment, except where individuals have consented to their data being accessed e.g. written consent for a research study. This is intended to give both GPs and patients a very high degree of confidence that their data will be safe and their privacy protected.
The TRE will be built in line with best practice developed in projects, such as OpenSAFELY and the Office for National Statistics’ Secure Research Service.
We are also committed to adopting a transparent approach, including publishing who has run what query and used which bit of data. We are developing a TRE which will meet our specific needs and act as “best in class”.
We commit to only begin the data collection once the TRE is in place. Further, we will ensure that the BMA, RCGP and the National Data Guardian have oversight of the proposed arrangements and are satisfied with them before data upload begins.
I can also confirm that the previously published Data Provision Notice for this collection has been withdrawn.
Once the data is collected, it will only be used for the purposes of improving health and care. Patient data is not for sale and will never be for sale.
Transparency, communications and engagement There has been a great deal of concern regarding the lack of awareness amongst the healthcare system and patients. We recognise that we need to strengthen engagement, including opportunities for non-digital engagement and communication. Since the programme has been paused, we have been developing an engagement and communications campaign, with the goal of ensuring that the healthcare system and patients are aware and understand what is planned, and can make informed choices. The public rightly look to and trust general practice - through a centrally driven communication campaign, with clear messages, we will seek to ensure that the introduction of this collection does not impose an additional burden on practices.
We are developing a communications strategy delivered through four phases.
● Listening - where we listen to stakeholders and gather views on how best to communicate with the profession, patients and the public and give them the opportunity to inform the development of the programme in areas such as opt-outs, trusted research environments and other significant areas;
● Consultation - a series of events where we can explain the programme, listen and capture feedback and co-design the information campaign;
● Demonstration - show how feedback is being used to develop the programme and shape communications to the healthcare system and the public;
● Delivery - of an information campaign to inform the healthcare system and the public about changes to how their GP data is used, that utilises the first three phases to ensure the campaign is accessible, has wide reach and is effective.
Data saves lives. The vaccine rollout for COVID-19 could not have been achieved without patient data. The discovery that the steroid Dexamethasone could save the lives of one third of the most vulnerable patients with COVID-19 – those on ventilators - could not have been made without patient data from GP practices in England. That insight has gone on to save a million lives around the globe. That is why this programme is so important.
The programme and I will be providing further information as the programme progresses. In the meantime, if you have any questions, you can contact the programme at enquiries@nhsdigital.nhs.uk. The NHS Digital web pages also provide further information at https://digital.nhs.uk/data-and-information/data-collections-and-data-sets/data-collections/general-practice-data-for-planning-and-research#additional-information-for-gp-practices.
Thank you for your continued support.
JO CHURCHILL
Parliamentary under Secretary of State for Primary Care and Health Promotion
Page created: 01 September 2020
